let’s take a look at Meningitis pathophysiology and other essential things for a better understanding of meningitis.
Meningitis is the inflammation of the lining (meninges) around the brain and spinal. Meninges are the three membranes that envelop the brain and spinal cord. In mammals, they are the dura mater, the arachnoid mater, and the pia mater.
Cerebrospinal fluid is located in the subarachnoid space between the arachnoid mater and the pia mater. The primary function of the meninges is to protect the central nervous system.
Overview of meningitis pathophysiology
In meningitis pathophysiology, it would be great to note that it affects all genders and ages and can spread easily among those living in close habitations.
If dealt with quickly, meningitis can be treated successfully. So it’s important to get routine vaccinations, know the first sign of meningitis, and get the right medical attention.
The swelling from meningitis typically triggers symptoms such as headache, fever, and a stiff neck.
This disorder could be a viral, bacterial, parasitic, or fungal infection. There are non-infectious causes of meningitis such as chemical reactions.
Meningitis pathophysiology
The Pathophysiology of meningitis is based on the type of the infection and the cause of meningitis.
Bacterial meningitis pathophysiology
- The systemic inflammatory response of the host leads to leukocyte extravasation into the subarachnoid space and increased CSF outflow resistance, and brain edema.
- Immune cells within the brain parenchyma, in particular microglia, can be stimulated by proinflammatory bacterial compounds, which can directly lead to neuronal injury.
- Some bacterial compounds, e.g., pneumolysin, possess direct toxicity on neurons. Neuronal injury is mediated by the release of reactive oxygen intermediates, proteases, cytokines, and excitatory amino acids, the activation of transcription factors, caspases, matrix metalloproteases, and other proteases.
- All these processes in meningitis pathophysiology bring about the symptoms observed in bacterial meningitis.
Viral meningitis pathophysiology
In viral meningitis pathophysiology, Viruses enter the CNS through several routes and mechanisms. For instance, enteroviruses, replicate outside the CNS and then invade by haematogenous spread. Viral particles pass directly across the blood-brain barrier, or are carried across in infected leukocytes, and then infect vascular endothelial cells.
Viruses may spread through the subarachnoid space in CSF, with consequent inflammatory response leading to meningitis. Viruses may also spread directly or via inflammatory leukocytes through neural tissue to neurones and glial cells.
Once CNS infection has taken hold, inflammatory cells, including lymphocytes specifically targeting the infecting virus, accumulate in the CNS.
This is accompanied by the release of inflammatory cytokines such as interleukin (IL)-1β, IL-6, and tumor necrosis factor (TNF)-α as well as local immunoglobulin production by plasma cells.
In the pathophysiology of viral meningitis, the Central Nervous System parenchyma is mostly involved, causing encephalitis.
Also, Communicating hydrocephalus which is a rare complication of viral meningitis and it is usually brought about by the obstruction of arachnoid granulations by inflammatory debris.
Fungal meningitis pathophysiology
The first phase of fungal meningitis is pulmonary exposure to the fungi by the inhalation of airborne fungal spores, which is followed by Inflammatory results leading to a primary pulmonary and lymph node focus limiting the inhaled organism from further spread. However, this stage might be without any sign or symptom of viral meningitis.
In most cases of fungal meningitis, the fungi undergo hematogenous spread, and Patients with immunosuppression are the most vulnerable to fungal meningitis. Once the fungi cross the blood-brain barrier they cause an inflammation of the meninges and arachnoid space.
The inflammation promotes cytokine release mainly tumor necrosis factor (TNF), interleukin 1, interleukin 2, interleukin 6, interleukin 12, colony-stimulating factors, and interferon-λ. The cytokines cause the fever observed in meningitis. The cytokines promote an increase in the permeability of the blood-brain barrier and subsequent cerebral edema and an increase in the intracranial pressure
Cerebral edema leads to decreased blood flow to the brain and hypoxia. The glucose level in the cerebral spinal fluid will decrease due to a decreased transport of glucose coupled to increased use of glucose by the fungi.
Parasitic meningitis pathophysiology
The pathophysiology of this type of meningitis is dependent on the different parasites that cause meningitis. Parasitic meningitis is also rare and the treatments are not specific.
Types of meningitis
Below are the different kinds of meningitis
- Viral meningitis
- Bacterial meningitis
- fungal meningitis
- parasitic meningitis
Viral meningitis
As the name implies it occurs because of a group of pathogenic viruses called enteroviruses. It can also be referred to as aseptic meningitis. Its occurrence is easier compared to bacterial meningitis but not usually life-threatening.
These enteroviruses could be mumps, herpes simplex virus, and others in that category.
Bacterial meningitis
In this case, bacteria may enter the bloodstream and travel to the brain and spinal cord where they irritate the meninges thereby causing acute bacterial meningitis.
Nevertheless, it can also occur when bacteria directly invade the meninges. An ear, sinus infection, or skull injury may cause this. It is usually rare but life-threatening. Bacterial meningitis is the most serious type of meningitis. It can lead to death or permanent disability. It is mostly regarded as a medical emergency.
It affects the meninges, the membranes that protect the central nervous system (CNS), together with the cerebrospinal fluid.
In 2006, the mortality rate for bacterial meningitis was 34 percent, and 50 percent of patients experienced long-term effects after recovery.
Below are some of the strains of bacteria that can cause acute bacterial meningitis
- Haemophilus influenzae (haemophilus). Haemophilus influenzae type b (Hib) bacterium was once the leading cause of bacterial meningitis in children.
- Streptococcus pneumoniae (pneumococcus). This bacterium is the most common cause of bacterial meningitis in infants, young children, and adults in the United States. It more commonly causes pneumonia or ear or sinus infections. A vaccine can help prevent this infection.
- Neisseria meningitidis (meningococcus).This bacterium is another leading cause of bacterial meningitis. These bacteria commonly cause an upper respiratory infection but can cause meningococcal meningitis when they enter the bloodstream. This is a highly contagious infection that affects mainly teenagers and young adults.
Fungal meningitis
Fungal meningitis is relatively uncommon and causes chronic meningitis. It may mimic acute bacterial meningitis.
Fungal meningitis isn’t contagious from person to person. Cryptococcal meningitis is a common fungal form of the disease that affects people with immune deficiencies, such as AIDS. It’s life-threatening if not treated with an antifungal medication.
What is the first sign of meningitis?
The first sign of meningitis can be any of the general signs of the disorder depending on different factors like age, immunity, and the cause of the disease.
General signs and symptoms of meningitis
Viral meningitis symptoms
Viral meningitis in infants may include:
- irritability
- decreased appetite
- fever
In adults, viral meningitis may cause:
- headaches
- stiff neck
- sensitivity to bright light
- lethargy
- nausea and vomiting
Bacterial meningitis symptoms
Bacterial meningitis symptoms develop suddenly. They may include:
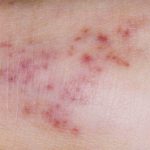
- Meningitis rash
- altered mental status
- nausea
- vomiting
- sensitivity to light
- irritability
- headache
- fever
- chills
- stiff neck
- purple areas of skin that resemble bruises
- sleepiness
- lethargy
Seek immediate medical attention if you experience these symptoms. Bacterial and viral meningitis can be deadly.
There is no way to know if you have bacterial or viral meningitis just by judging how you feel. Your doctor will need to perform tests to determine which type you have.
Fungal meningitis symptoms
Symptoms of fungal meningitis resemble the other types of this infection. These may include:
- nausea
- vomiting
- sensitivity to light
- fever
- headache
- confusion or disorientation
Is meningitis contagious?
Several types of meningitis are not contagious. Fungal, parasitic, and non-infectious meningitis is not contagious.
Viral meningitis is contagious. It’s spread through direct contact with body fluids, including mucus, feces, and saliva.
Droplets of infected fluid can be spread and shared with sneezing and coughing. You do not have to come into direct contact with an infected person to pick up this infection.
Bacterial meningitis, the most serious form of meningitis, can also be contagious, especially if it’s meningococcal meningitis.
It’s spread through extended contact with an infected person. Schools, daycare centers, military barracks, hospitals, and college dormitories are prime locations for sharing this infection.
How is meningitis diagnosed?
Diagnosing meningitis starts with a health history and physical exam. During the physical exam, your doctor will look for:
- a fever
- an increased heart rate
- neck stiffness
- reduced consciousness
Your doctor will also order a lumbar puncture. This test is also called a spinal tap.
It allows your doctor to look for increased pressure in the central nervous system. It can also find inflammation or bacteria in the spinal fluid. This test can also determine the best antibiotic for treatment.
Other tests may also be ordered to diagnose meningitis. Common tests include the following:
- Blood cultures identify bacteria in the blood. Bacteria can travel from the blood to the brain. N. meningitidis and S. pneumonia, among others, can cause both sepsis and meningitis.
- A complete blood count with differential is a general index of health. It checks the number of red and white blood cells in your blood. White blood cells fight infection. The count is usually elevated in meningitis.
- Chest X-rays can reveal the presence of pneumonia, tuberculosis, or fungal infections. Meningitis can occur after pneumonia.
- A CT scan of the head may show problems like a brain abscess or sinusitis. Bacteria can spread from the sinuses to the meninges.
Is meningitis preventable?
These steps can help prevent meningitis:
- Wash your hands. Careful hand-washing helps prevent the spread of germs.
- Practice good hygiene. Don’t share drinks, foods, straws, eating utensils, lip balms, or toothbrushes with anyone else. Teach children and teens to avoid sharing these items too.
- Stay healthy. Maintain your immune system by getting enough rest, exercising regularly, and eating a healthy diet with plenty of fresh fruits, vegetables, and whole grains.
- Consider being vaccinated
Recommendations
what is a pathogen? and the 4 main pathogens
Can you join the military with ADHD?
Iron Deficiency Anemia: Symptoms, Causes, and Treatment
How Serious Is NASH? All You Need To Know About This Silent Liver Disease



One comment